Guest post by Erik Messamore, MD, Johnny’s Ambassadors Scientific Advisory Board member
This article was originally published on Dr. Messamore’s blog.
PSYCHOSIS IS ONE OF THE OLDEST AND BEST-DOCUMENTED RISKS OF CANNABIS USE.
Associations between cannabis use and psychosis appeared in the medical literature soon after cannabis was introduced into Western medical practice in the 1850s. Physicians of the 19thcentury accurately identified marijuana’s therapeutic value. Medical textbooks and journals of that era described benefits in the treatment of pain, epilepsy, the sundowning phenomenon in dementia, muscle spasticity, menstrual pain, and other types of pain. So, our 19th-century predecessors accurately recognized the benefits that are being claimed in the 21st century. They also accurately described the risk of psychosis. Yet many today are unaware that cannabis poses any such risk.
CONSISTENT ASSOCIATION
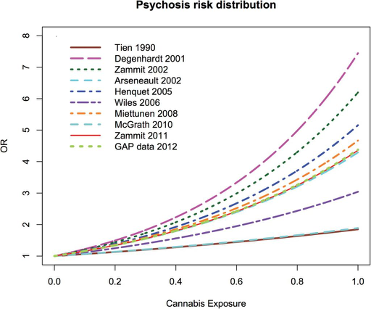
No less than ten different peer-reviewed studies have shown strong correlation between the degree of cannabis exposure in earlier-life and the risk of schizophrenia in later-life. The risk of schizophrenia among regular cannabis users rises by an average of 300%. Some have reported a nearly 700% increased risk. This figure from Arianna Marconi and collaborators, published in Schizophrenia Bulletin, sums up the status of the findings as of 2016.
BUT DOES IT PROVE CAUSATION?
Showing that two things are correlated does not necessarily prove that one causes the other. Some cannabis proponents will emphasize this point, presumably to deflect the obvious concerns.
The only way to definitely prove that regular cannabis use does (or does not) cause schizophrenia would be to round up about 10,000 people who never used cannabis and randomly assign half to regularly use cannabis and half to regularly use some appropriate placebo cannabis. And then count the new cases of persistent psychosis over the next 10 years. Obviously, the definitive experiment can never be done. Incidentally, we never did this type of study to establish the causative link between earlier-life cigarette use and later-life cancer.
When the outcomes are potentially dangerous, we draw conclusions (and make health advisories) based on probable cause. We establish probable cause by looking for: biochemical plausibility, the ability to model the outcome in animals, and significant correlation between the extent of exposure and the likelihood of the outcome in human populations. All these criteria have been satisfied for the cannabis-schizophrenia connection.
THE CENTRAL FEATURE OF PSYCHOSIS OR SCHIZOPHRENIA
Schizophrenia is a condition of persistent psychosis, and the heart of psychosis is misperception. Consistently misperceived external events or frequent misperception of internal thoughts or feelings are the building blocks of psychosis. People enjoy using cannabis precisely because it causes the brain to register misperceptions (of time, sensation, emotion, or significance of one’s thoughts). It should not be too difficult to see how it triggers psychosis.
BIOCHEMICAL PLAUSIBILITY FOR CANNABIS TO CAUSE PSYCHOSIS OR SCHIZOPHRENIA
The pharmacology of cannabis substantially overlaps with the neurochemistry of psychosis or schizophrenia.
Dopamine is clearly relevant to psychosis and schizophrenia. The brain uses dopamine to create perceptions of significance to external events – or to internal thoughts or feelings. The mind begins to create special beliefs that can explain these perceptions of improbable significance. Cannabis substantially alters dopamine release and sensitivity. Affecting dopamine signaling is one way that cannabis can cause psychosis or schizophrenia.
Glutamate is another well-known schizophrenia-related neurotransmitter. More than half of the nerve cells in the brain use glutamate to communicate with each other. In terms of the number of connections utilizing it, glutamate is the brain’s leading neurotransmitter. Glutamate is especially important in the networks of the cerebral cortex that form complex perceptions. It’s no surprise, then, that drugs that interfere with glutamate can cause psychosis. Ketamine and PCP are two noteworthy examples. Defective glutamate signaling is a frequent finding in schizophrenia. Meanwhile one of the major actions of cannabis is to inhibit glutamate release throughout the brain.
Data suggest that anandamide is anti-inflammatory in the brain and is neuroprotective. Cannabis users have lower anandamide levels, in line with the expectation that exogenous cannabinoids suppress endogenous cannabinoids. Meanwhile, it appears that anandamide may protect against schizophrenia. Suppressing anandamide levels by regularly using cannabis may remove this protection. Suppressing anti-inflammatory anandamide by cannabis is also a concern because many cases of schizophrenia are provoked by inflammation.
Finally, regular cannabis use could lead to persistent psychosis by making the brain hypersensitive to serotonin. Recent data show that daily THC in adolescence sensitizes the serotonin 2A receptor of rodents. This is significant because this particular serotonin receptor is the main target of LSD.
CREATING THE NEUROPHYSIOLOGY OF SCHIZOPHRENIA IN ANIMALS
Not only can cannabis create the neurochemical conditions for psychosis or schizophrenia, but we can also show that it causes schizophrenia-like effects in animals. Most people believe schizophrenia to be a disease of the mind. But psychosis is a neurological symptom and schizophrenia is an illness of the brain. Because it’s a brain condition, it has signs that can be detected in the laboratory. We can observe these signs in animals as well. And scientists have used animal models of schizophrenia both to learn more about the illness in humans and to discover treatments. Exposing animals to cannabis, or to its major chemical component THC, causes a number of schizophrenia-like changes in brain function. Here is a summary of animal studies showing schizophrenia-like changes from cannabinoid exposure.
BUT SCHIZOPHRENIA RATES AREN’T CHANGING… OR ARE THEY?
The data linking cannabis use to higher risk of schizophrenia are so solid that most proponents don’t dispute them. At worst, they argue, it may accelerate the onset of symptoms in people already destined to develop schizophrenia. They ask: if cannabis causes schizophrenia, why don’t we see higher rates of schizophrenia in places where it’s used more frequently? Often, these arguments rely on the belief that schizophrenia rates are relatively constant across the globe. There are two problems with this.
First, the incidence of schizophrenia does vary across geography and over time. To my knowledge, however, no one has studied the incidence (rate of new cases) of schizophrenia in validly-comparable regions where cannabis use is prevalent versus where it’s rare.
Second, our ability to detect changes in the incidence of schizophrenia is poor. I’m not aware of any systems in the USA that allow for accurate capture of data on new cases of schizophrenia. Even the NIH appears to have a devilishly hard time knowing how many people in the USA have schizophrenia. There is also the problem of time-lag. Like the cigarette-cancer relationship, the cannabis-schizophrenia relationship takes years to observe. If we were able accurately track new diagnoses of schizophrenia in cannabis-friendly Colorado and compare them to its cannabis-unfriendly border state of Kansas, we would have to wait many years for the impact to be measurable.
Using the incidence/prevalence argument to argue that cannabis doesn’t cause schizophrenia is tough. It’s really hard to get the kind of data accuracy to convincingly support it.
Without a doubt, some portion of the link between earlier-life cannabis use and later-life schizophrenia risk comes from the acceleration of symptoms in those predestined to express them. However, there is a really good case to be made for the likelihood that regular cannabis use can cause schizophrenia-like illness de novo. In other words, regular cannabis use across a population probably does increase the number of schizophrenia cases above the natural background. We should make sure people know this.
THERE IS ENOUGH PROBABLE CAUSE TO MAKE THIS A PUBLIC HEALTH PRIORITY
We should not wait for the perfect studies to “prove” that the cannabis-schizophrenia risk has enough validity to start warning consumers. First, the only definitive proof would have to come from the kind of studies that cannot ethically (or practically) be conducted. Second, there is no such thing as the perfect study. Conclusions in science are based on many types of evidence with logical connections between them. And finally, with significant money to be made in the cannabis trade, there will always be a number of critics who say we need more data. Those critics, in many cases, will have substantial advertising and PR budgets. Meanwhile, psychosis is a severe adverse effect and schizophrenia is a long term and devastating (and very expensive) outcome. We have credible science showing probable cause. Prudence (and common sense) demands that the public know about the risk.
Others have also argued that regular use of cannabis probably does cause psychosis. Professor Jonathan K. Burns, makes the case in an excellent review in Frontiers in Psychiatry. More recently, neuroscientist Christine L. Miller penned a well-referenced article where she concludes:
“The causal link between marijuana use and the development of psychosis is quite simply the most well-replicated, high-impact finding in schizophrenia research today… it stands to be responsible for a larger proportion of schizophrenia cases than any other established factor.”
I join Dr. Miller in calling for the surgeon general, neuroscientists, psychiatrists, and professional societies to inform the public about this risk. And for journalists to pay heed.
The government of Canada used to require all marijuana packaging to carry specific warnings about credible health risks. Among these warnings is the statement – backed by abundant science – that cannabis can increase the risk of psychosis and schizophrenia. It’s time we have similar warnings in the USA.



